Click here to download the PDF.


In the two previous articles on Lyme disease we explained the importance of prevention and prompt treatment of early Lyme disease. What happens if an individual is not treated promptly?
Lyme disease is a bacterial infection transmitted by mostly the Deer tick. When a tick bites, it injects the individual with the Lyme disease bacteria. The bacteria travel through the skin and enter veins to circulate throughout the body and deposit it in specific target organs. These may include muscles, tendons and ligaments and joints, leading to the flu-like symptoms many individuals describe. If not treated or not cured at this early stage the final target organ of this germ is the Brain.
Unfortunately, there is no oral antibiotic that can cross the blood-brain effectively to kill this bacterium in the brain. This is the reason that oral antibiotic therapy for Lyme disease is not universally effective in treating early disease. If even a few bacteria get to the brain before oral antibiotic therapy is started, the individual will not be cured of Lyme disease and will develop a different presentation of Lyme disease called Late stage Lyme disease.
These individuals may in fact appear to get well from the initial oral antibiotic treatment, but somewhere within three months to a year after treatment may begin to develop new signs and symptoms. This may include more classic signs and symptoms such as swollen joints, but many will begin to experience more slowly progressive issues that may come and go. These may include fatigue, headaches, muscle and joint pains, Bell’s palsy, dizziness, memory problems, confusion, shooting pains, behavioral changes such as depression to name just a few. In fact Lyme disease has mimicked many other diseases.
Late stage Lyme disease, treatment requires the use of intravenous antibiotics as these are the only agents which can cross the brains’ blood-brain barrier at dosages which are adequate to kill the Lyme disease bacteria. Prior to embarking on this treatment the Physician should confirm that the individual is really infected with the Lyme disease bacterium. What we consider sound medical practice to achieve this goal will be described in next week’s installment.
 Fall is here! It’s time to start putting away yard equipment, watch the kids participate in outdoor sporting events or a stroll through the many scenic parks or wooded neighborhoods throughout Pennsylvania, New Jersey, Maryland, Delaware, and New York. It’s also tick season. Yes, even they have a season.
Fall is here! It’s time to start putting away yard equipment, watch the kids participate in outdoor sporting events or a stroll through the many scenic parks or wooded neighborhoods throughout Pennsylvania, New Jersey, Maryland, Delaware, and New York. It’s also tick season. Yes, even they have a season.
Early to late spring and fall are the times when ticks emerge looking for a blood meal. The tick most often associated with Lyme disease is the deer tick, though all ticks can carry a number of other diseases that can be transmitted to humans. Deer ticks are small, about the size of a pinhead, making them difficult to find once attached. Other ticks such as the dog tick and the Lone Star tick are larger, but can infect you more quickly than the deer tick.
Lyme disease ticks waiting in the bush
Ticks are found in low-lying brush, grass or shrubs, and will attach to the unaware host as he or she walks by. Ticks crawl upward on their host until they reach an impediment to their progress that they cannot overcome. Common areas of attachment are behind the knee, groin, waistline, armpit, or scalp. They attach by piercing the skin with a mouthpiece after secreting an anesthetic from their salivary gland. Attaching pain free, in an out of sight area is how the ticks avoid detection. Once attached, blood is siphoned from the host, mixed in the tick’s mid-gut and the tick regurgitated back into the host. The tick may need to be attached for up to 24 hours for the person to be infected, but it can occur even within a few hours.
Caution when removing deer tick
It is important that when a tick is removed that it is not crushed or burned. It should be grasped firmly by its mouthpiece with a forceps and pulled out. If part of the mouthpiece remains in your skin, consult with a physician for further removal. There is no effective means of immediately identifying an infected Deer tick from an uninfected one at the time of removal. The onset of symptoms can vary and may be delayed. It is currently recommended that all patients who have a Deer tick bite should receive preventive antibiotic therapy, so taking a wait-and-see attitude before reporting it to your family physician can be dangerous.
Lyme disease symptoms are divided into two distinct stages called Early and Late disease. Early localized disease often starts with flu-like feelings of headache, muscle and joint and neck stiffness, low-grade fever and fatigue. Less than 80 percent of patients develop an Erythema Migraines rash or “Bulls Eye” rash. This rash is proof of Lyme disease and always occurs at the bite site. It appears anywhere from 3 days to 3weeks after an exposure, expands outward from a clear center with red outer border and may or may not be accompanied by other symptoms. This rash typically lasts 2-4 weeks and disappears on its own. While a physician can confirm a case of Early Lyme disease with this finding, it is the least common type of rash that occurs with Lyme disease! Taking a picture of the rash before it disappears is extremely important in helping your physician to make an accurate diagnosis.
Symptoms associated with Early and Late Lyme Disease are Bell’s Palsy, tingling sensations of the upper and lower extremities, severe headaches, problems with short term memory, diminished concentration and speech disturbances. Other complaints may be visual disturbances, neck stiffness, cardiac or pulmonary complaints, chronic fatigue, insomnia, depression or anxiety issues.
Lyme testing
Testing for Lyme disease is traditionally performed using two tests called the ELISA and Western Blot. When positive they can confirm a case of Lyme disease, but they can be negative in up to 7 out of 10 patients who are truly infected. There are newer tests such as the C6 Peptide ELISA for Lyme disease and PCR, a genetic test, which can assist the physician in making the diagnosis in more difficult to diagnose patients. (See Accurate Lyme Diagnosis)
Fortunately, the Haverford Wellness Center under the direction of Domenic Braccia D.O. is dedicated to the accurate diagnosis and reasonable treatment of Lyme disease and other tick borne diseases. Dr. Braccia, and the sof the Haverford Wellness Center are fully equipped and capable of managing aspects of Lyme disease and the other tick borne diseases from prevention and management of early disease to the complex diagnostic and therapeutic cases. These cases include treatment failures, and late stage Lyme disease patients who have been ill for many years.
 The Lyme disease bacterium, Borrelia burgdorferi, normally lives in mice, squirrels and other small animals. It is transmitted among these animals and to humans through the bites of certain species of ticks. In the northeastern and north-central United States, the black-legged tick (or deer tick, Ixodes scapularis) transmits Lyme disease. In the Pacific coastal United States, the disease is spread by the western black-legged tick (Ixodes pacificus). Other major tick species found in the United States have not been shown to transmit Borrelia burgdorferi.
The Lyme disease bacterium, Borrelia burgdorferi, normally lives in mice, squirrels and other small animals. It is transmitted among these animals and to humans through the bites of certain species of ticks. In the northeastern and north-central United States, the black-legged tick (or deer tick, Ixodes scapularis) transmits Lyme disease. In the Pacific coastal United States, the disease is spread by the western black-legged tick (Ixodes pacificus). Other major tick species found in the United States have not been shown to transmit Borrelia burgdorferi.
Blacklegged ticks transmit Lyme disease
Blacklegged (or deer) ticks (Ixodes scapularis and Ixodes pacificus) can transmit several tick-borne diseases including anaplasmosis, babesiosis and Lyme disease. An adult tick is pictured at left, though it is the smaller nymphal stage ticks which most commonly bite humans.
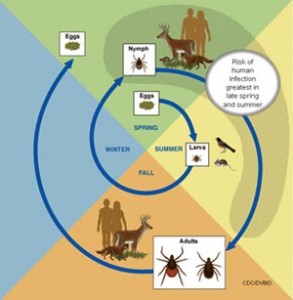 Life cycle of blacklegged ticks
Life cycle of blacklegged ticks
Blacklegged ticks live for two years and have three feeding stages: larvae, nymph, and adult. Tick eggs are Tick Lyme Disease Treatmentlaid in the spring and hatch as larvae in the summer. Larvae feed on mice, birds, and other small animals in the summer and early fall. When a young tick feeds on an infected animal, the tick takes bacteria into its body along with the blood meal, and it remains infected for the rest of its life. After this initial feeding, the larvae become inactive as they grow into nymphs. The following spring, nymphs seek blood meals in order to fuel their growth into adults. When the tick feeds again, it can transmit the bacterium to its new host. Usually the new host is another small rodent, but sometimes the new host is a human. Most cases of human illness occur in the late spring and summer when the tiny nymphs are most active and human outdoor activity is greatest. Adult ticks feed on large animals, and sometimes on humans. In the spring, adult female ticks lay their eggs on the ground, completing the life cycle. Although adult ticks often feed on deer, these animals do not become infected. Deer are nevertheless important in transporting ticks and maintaining tick populations.
Early Lyme diagnosis and Lyme treatment are critical to a successful cure.
Avoid areas with a lot of ticks
Keep ticks off your skin
Check your skin and clothes for ticks every day
If you suspect Lyme disease it’s important to get an accurate diagnosis and Lyme treatment started right away.
 Insect repellant for ticksSawyer not only repels insects, it actually kill ticks, mosquitoes, chiggers, mites and more than 100 other kinds of insects. Sawyer repellents are for use on clothing, tents and other gear only. A single application will remain effective for up to six weeks, even if you wash the garment once a week.
Insect repellant for ticksSawyer not only repels insects, it actually kill ticks, mosquitoes, chiggers, mites and more than 100 other kinds of insects. Sawyer repellents are for use on clothing, tents and other gear only. A single application will remain effective for up to six weeks, even if you wash the garment once a week.
Visit the Sawyer website for more information or to purchase
 Medical Doctor at Haverford Wellness Center
Medical Doctor at Haverford Wellness Center 1. Recent infection before immune response
1. Recent infection before immune response
2. Antibodies are in immune complexes
3. Spirochete encapsulated by host tissue (i.e.: lymphocytic cell walls)
4. Spirochete is deep in host tissue (i.e.: fibroblasts, neurons, etc.)
5. Blebs in body fluid, no whole organisms available for PCR
6. No spirochetes in body fluid on day of test
7. Genetic heterogeneity (300 strains, 100 in U.S.)
8. Antigenic variability
9. Surface antigens change with temperature
10. Utilization of host protease instead of microbial protease
11. Spirochete in dormancy phase (L-form) with no cell walls Additional Reasons for False Lyme test
12. Recent antibiotic treatment
13. Recent anti-inflammatory treatment
14. Concomitant infection with babesia may cause immunosuppression
15. Other causes of immunosuppression
16. Lab with poor technical capability for Lyme disease
17. Lab tests not standardized for late stage disease
18. CDC criteria is epidemiological not a diagnostic criteria
19. Lack of standardized control
20. Most controls use only a few strains as reference point
21. Few organisms are sometimes present
22. Encapsulated by glycoprotein “S-layer” which impairs immune recognition
23. “S”- layer binds to IgM
24. Immune deficiency
25. Possible down regulation of immune system by cytokines
26. Revised Western Blot test criteria fails to include most significant antigens